Abstract
Background
Anticoagulation therapy with warfarin is widely considered the standard of care for stoke prophylaxis in patients with atrial fibrillation who are at high risk of stroke. Community-based studies in the US have reported that the effectiveness of anticoagulation varies by management approach and that patients receiving warfarin have international normalised ratio (INR) values within the target therapeutic range less than half the time.
Objective
To estimate the lifetime societal costs and health benefits of warfarin therapy to prevent strokes, specifically in elderly patients (mean age 70 years) with atrial fibrillation who are at high risk of stroke, when anticoagulation is managed through usual care versus anticoagulation management services, where dedicated anticoagulation professionals (e.g. physician or pharmacist) monitor and oversee patients.
Methods
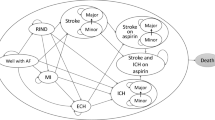
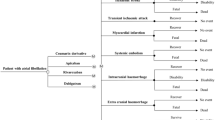
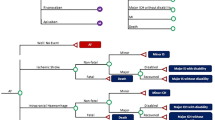
Semi-Markov decision model with a 30-day cycle length and 10-year time horizon (to reflect the mean life expectancy of the study population). Univariate sensitivity analyses and Bayesian second-order multivariate probabilistic sensitivity analysis using Monte Carlo simulation were performed.
Outcomes measures were costs and QALYs. Most of the probability and outcome estimates included were derived from the recent SPORTIF (Stroke Prevention using ORal Thrombin Inhibitor in atrial Fibrillation) V trial. Utility values were derived from a large, nationally representative sample of individuals in the Medical Expenditure Panel Survey and were adjusted for age, sex, race, ethnicity, income, education and co-morbidity. Resource utilisation was based on experience at the University Medicine Group Practice Anticoagulation Clinic (University of Colorado, Denver, CO, USA) and costs ($US; 2004 values) included were for warfarin and aspirin (acetylsalicylic acid) use and those associated with major bleeding, treatment of primary events, routine INR and biochemistry monitoring, ECGs, and clinic visits. Costs and outcomes were discounted by 3% per annum.
Results
The anticoagulation management service improved effectiveness by 0.057 (95% credible interval 0, 0.36) QALYs and reduced costs by $US2100 (95% credible interval −$US19 800, $US300) [2004 values] compared with usual care. Results were sensitive to the extent of the increase in risk of primary events (all strokes and systemic embolic events attributable to usual care, but were robust to variation in other input variables). The anticoagulation management service was the dominant strategy in 91% of Monte Carlo simulations.
Conclusion
The anticoagulation management service appears to cost less and provide greater effectiveness than usual care. To enhance stroke prophylaxis among high-risk patients with atrial fibrillation, physicians and Medicare plans may wish to consider augmenting ‘usual care’ by the addition of patient-monitoring technology strategies such as formally organised anticoagulation monitoring programmes.



Similar content being viewed by others
References
Hart RG, Halperin JL, Pearce LA, et al. Lessons from the stroke prevention in atrial fibrillation trials. Ann Intern Med 2003 May 20; 138 (10): 831–838
Wolf PA, Abbott RD, Kannel WB. Atrial fibrillation as an independent risk factor for stroke: the Framingham Study. Stroke 1991 Aug; 22 (8): 983–988
Ryder KM, Benjamin EJ. Epidemiology and significance of atrial fibrillation. Am J Cardiol 1999 Nov 4; 84 (9A): 131R–138R
Albers GW, Dalen JE, Laupacis A, et al. Antithrombotic therapy in atrial fibrillation. Chest 2001 Jan; 119 (1 Suppl.): 194S–1206S
Lip GY, Beevers DG. ABC of atrial fibrillation: history, epidemiology, and importance of atrial fibrillation. BMJ 1995 Nov 18; 311 (7016): 1361–1363
Hylek EM, Skates SJ, Sheehan MA, et al. An analysis of the lowest effective intensity of prophylactic anticoagulation for patients with nonrheumatic atrial fibrillation. N Engl J Med 1996 Aug 22; 335 (8): 540–546
Fang MC, Chang Y, Hylek EM, et al. Advanced age, anticoagulation intensity, and risk for intracranial hemorrhage among patients taking warfarin for atrial fibrillation. Ann Intern Med 2004 Nov 16; 141 (10): 745–752
Holbrook AM, Pereira JA, Labiris R, et al. Systematic overview of warfarin and its drug and food interactions. Arch Intern Med 2005 May 23; 165 (10): 1095–1106
Ansell JE. Optimizing the efficacy and safety of oral anticoagulant therapy: high-quality dose management, anticoagulation clinics, and patient self-management. Semin Vasc Med 2003 Aug; 3 (3): 261–270
Samsa GP, Matchar DB, Goldstein LB, et al. Quality of anticoagulation management among patients with atrial fibrillation: results of a review of medical records from 2 communi-ties. Arch Intern Med 2000 Apr 10; 160 (7): 967–973
Matchar DB, Samsa GP, Cohen SJ, et al. Improving the quality of anticoagulation of patients with atrial fibrillation in managed care organisations: results of the managing anticoagulation services trial. Am J Med 2002 Jul; 113 (1): 42–51
Witt DM, Sadler MA, Shanahan RL, et al. Effect of a centralized clinical pharmacy anticoagulation service on the outcomes of anticoagulation therapy. Chest 2005 May; 127 (5): 1515–1522
Caro JJ. An economic model of stroke in atrial fibrillation: the cost of suboptimal oral anticoagulation. Am J Manag Care 2004 Dec; 10 (14 Suppl.): S451–S458; discussion S458-61
Locke C, Ravnan SL, Patel R, et al. Reduction in warfarin adverse events requiring patient hospitalization after implementation of a pharmacist-managed anticoagulation service. Pharmacotherapy 2005 May; 25 (5): 685–689
Lafata JE, Martin SA, Kaatz S, et al. The cost-effectiveness of different management strategies for patients on chronic warfarin therapy. J Gen Intern Med 2000 Jan; 15 (1): 31–37
Chiquette E, Amato MG, Bussey HI. Comparison of an anticoagulation clinic with usual medical care: anticoagulation control, patient outcomes, and health care costs. Arch Intern Med 1998 Aug 10–24; 158 (15): 1641–1647
Olsson SB. Stroke prevention with the oral direct thrombin inhibitor ximelagatran compared with warfarin in patients with non-valvular atrial fibrillation (SPORTIF III): randomised controlled trial. Executive Steering Committee on behalf of the SPORTIF III Investigators. Lancet 2003 Nov 22; 362 (9397): 1691–1698
Albers GW, Diener HC, Frison L, et al. Ximelagatran vs warfarin for stroke prevention in patients with nonvalvular atrial fibrillation: a randomized trial. JAMA 2005 Feb 9; 293 (6): 690–698
National Center for Health Statistics US. Chartbook on trends in the health of americans [online]. Available from URL: http:// www.cdc.gov/nchs/data/hus/hus04trend.pdf#027 [Accessed2005 Apr]
Wolf PA, Mitchell JB, Baker CS, et al. Impact of atrial fibrillation on mortality, stroke, and medical costs. Arch Intern Med Feb 9 1998; 158 (3): 229–234
Greenlee RT, Vidaillet H. Recent progress in the epidemiology of atrial fibrillation. Curr Opin Cardiol 2005 Jan; 20 (1): 7–14
Miyasaka Y, Barnes ME, Gersh BJ, et al. Time trends of ischemic stroke incidence and mortality in patients diagnosed with first atrial fibrillation in 1980 to 2000: report of a community-based study. Stroke 2005 Nov; 36 (11): 2362–2366
Benjamin E, Wolf P, D’Agostino R, et al. Impact of atrial fibrillation in the risk of death: the Framingham Heart Study. Circulation 1998; 98: 946–952
Hart RG, Benavente O, McBride R, et al. Antithrombotic therapy to prevent stroke in patients with atrial fibrillation: a meta-analysis. Ann Intern Med 1999; 131: 492–501
Johnson CE, Lim WK, Workman BS, et al. People aged over 75 in atrial fibrillation on warfarin: the rate of major hemorrhage and stroke in more than 500 patient-years of follow-up. J Am Geriatr Soc 2005 Apr; 53 (4): 655–659
O’Brien CL, Gage BF. Costs and effectiveness of ximelagatran for stroke prophylaxis in chronic atrial fibrillation. JAMA 2005 Feb 9; 293 (6): 699–706
Sullivan PW, Lawrence Jr WF, Ghushchyan V. A national catalogue of preference-based scores for chronic conditions in the U.S. Medical Care 2005; 43 (7): 736–749
Drugstore.com [online]. Available from URL: http://www.drugstore.com. [Accessed 2005 Jan 16]
Agency for Healthcare Research and Quality (AHRQ). HCUP database [online]. Available from URL: http://hcup.ahrq.gov/ HCUPnet.asp [Accessed 2005 Apr]
Youman P, Wilson K, Harraf F, et al. The economic burden of stroke in the United Kingdom. Pharmacoeconomics 2003; 21 Suppl. 1: 43–50
Caro JJ, Huybrechts KF. Stroke treatment economic model (STEM): predicting long-term costs from functional status. Stroke 1999 Dec; 30 (12): 2574–2579
Payne KA, Huybrechts KF, Caro JJ, et al. Long term cost-of-illness in stroke: an international review. Pharmacoeconomics 2002; 20 (12): 813–825
Centers for Medicare and Medicaid Services. U.S. Department of Health and Human Services. Clinical laboratory fee schedule [online]. Available from URL: http://www.cms.hhs.gov/ ClinicalLabFeesched/02_clinlab.asp [Accessed 2005 Jan 15]
Hart RG, Pearce LA, Koudstaal PJ. Transient ischemic attacks in patients with atrial fibrillation: implications for secondary prevention. The European Atrial Fibrillation Trial and Stroke Prevention in Atrial Fibrillation III trial. Stroke 2004 Apr; 35 (4): 948–951
Daffertshofer M, Mielke O, Pullwitt A, et al. Transient ischemic attacks are more than ‘ministrokes’. Stroke 2004 Nov; 35 (11): 2453–2458
Hill MD, Yiannakoulias N, Jeerakathil T, et al. The high risk of stroke immediately after transient ischemic attack: a population-based study. Neurology 2004 Jun 8; 62 (11): 2015–2020
CMS. Medicare Provider Analysis and Review (MEDPAR) of short-stay hospitals [online]. Available from URL: http:// www.cms.hhs.gov/statistics/medpar/default.asp [Accessed 2005 Jan 15]
US Bureau of Labor Statistics. Series I.D.# CUUR0000SAM, medical care [online]. Available from URL: http://data.bls.gov/cgi-bin/surveymost [Accessed 2005 Jan 15]
Gold MR, Siegel JE, Russell LB, et al., editors. Cost-effective-ness in health and medicine. New York: Oxford University Press, 1996
Menzin J, Boulanger L, Hauch O, et al. Quality of anticoagulation control and costs of monitoring warfarin therapy among patients with atrial fibrillation in clinic settings: a multisite managed-care study. Ann Pharmacother 2005 Mar; 39 (3): 446–451
Sullivan PW, Ghushchyan V. Preference-based EQ-5D index scores for chronic conditions in the U.S. Med Decis Making 2006; 26 (4): 410–420
Gage BF, Cardinalli AB, Owens DK. The effect of stroke and stroke prophylaxis with aspirin or warfarin on quality of life. Arch Intern Med 1996 Sep 9; 156 (16): 1829–1836
Briggs AH. Handling uncertainty in cost-effectiveness models. Pharmacoeconomics 2000 May; 17 (5): 479–500
Briggs AH, Goeree R, Blackhouse G, et al. Probabilistic analysis of cost-effectiveness models: choosing between treatment strategies for gastroesophageal reflux disease. Med Decis Making 2002 Jul–Aug; 22 (4): 290–308
Weinstein MC, Toy EL, Sandberg EA, et al. Modeling for health care and other policy decisions: uses, roles, and validity. Value Health 2001 Sep–Oct; 4 (5): 348–361
Fang MC, Stafford RS, Ruskin JN, et al. National trends in antiarrhythmic and antithrombotic medication use in atrial fibrillation. Arch Intern Med 2004 Jan 12; 164 (1): 55–60
Currie CJ, Jones M, Goodfellow J, et al. Evaluation of survival and ischaemic and thromboembolic event rates in patients with non-valvar atrial fibrillation in the general population when treated and untreated with warfarin. Heart 2006 Feb; 92 (2): 196–200
Pengo V, Pegoraro C, Cucchini U, et al. Worldwide management of oral anticoagulant therapy: the ISAM study. J Thromb Thrombolysis 2006 Feb; 21 (1): 73–77
Samsa GP, Matchar DB, Phillips DL, et al. Which approach to anticoagulation management is best? Illustration of an interactive mathematical model to support informed decision making. J Thromb Thrombolysis 2002 Oct; 14 (2): 103–111
Yousef ZR, Tandy SC, Tudor V, et al. Warfarin for nonrheumatic atrial fibrillation: five year experience in a district general hospital. Heart 2004 Nov; 90 (11): 1259–1262
Hambleton J. Home monitoring of anticoagulation. J Thromb Thrombolysis 2003 Aug–Oct; 16 (1–2): 39–42
Menendez-Jandula B, Souto JC, Oliver A, et al. Comparing self-management of oral anticoagulant therapy with clinic management: a randomized trial. Ann Intern Med 2005 Jan 4; 142 (1): 1–10
Wittkowsky AK, Sekreta CM, Nutescu EA, et al. Barriers to patient self-testing of prothrombin time: national survey of anticoagulation practitioners. Pharmacotherapy 2005 Feb; 25 (2): 265–269
Miller PS, Andersson FL, Kalra L. Are cost benefits of anticoagulation for stroke prevention in atrial fibrillation underestimated? Stroke 2005 Feb; 36 (2): 360–366
Acknowledgements
This research was supported by an unrestricted grant from The Bristol Myers Squibb Company. The authors had complete autonomy in all aspects of study design and conduct and manuscript preparation. The authors have no conflicts of interest that are directly relevant to the content of this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sullivan, P.W., Arant, T.W., Ellis, S.L. et al. The Cost Effectiveness of Anticoagulation Management Services for Patients with Atrial Fibrillation and at High Risk of Stroke in the US. Pharmacoeconomics 24, 1021–1033 (2006). https://doi.org/10.2165/00019053-200624100-00009
Published:
Issue Date:
DOI: https://doi.org/10.2165/00019053-200624100-00009